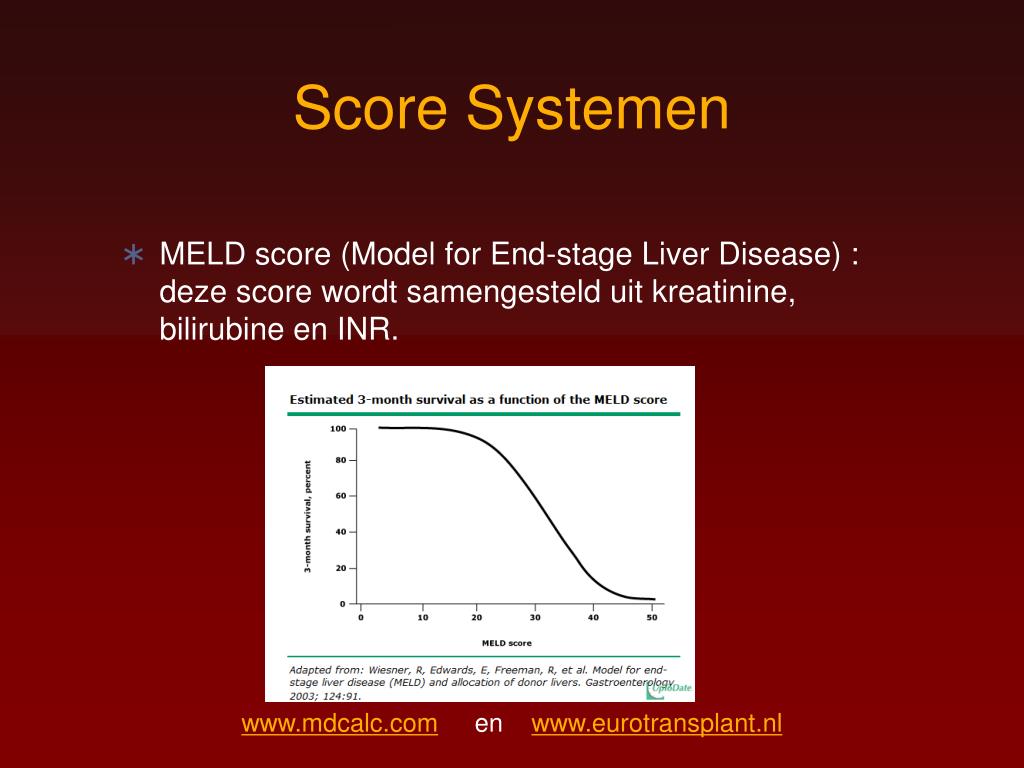
Most transplant patients follow their MELD scores and have a general idea of where they stand on the waiting list. In the case of living donor liver transplant, your medical team may still calculate a MELD score and place you on the transplant waiting list, but the time of your transplant will be determined by your doctors, not by your score on the waiting list. Liver allocation is a complex process, and MELD score is just one of the variables doctors use to determine who receives the next available liver. Remember, not every liver goes to the first person on the waiting list. Your position on the waiting list can change quickly, and your care team keeps close track of these numbers and will let you know when you are near the top of the list. These exceptions rarely happen, but in some cases, the review board will grant a higher score. In case of a medical condition that is not covered by the MELD score, if your care team believes your case qualifies for an exception, they can submit information to a review board and request a higher score. In some cases there may be special circumstances such as certain liver cancers that are not taken into account during your score calculation. These results are entered into a mathematical formula using the UNOS MELD score calculator. Your MELD score is calculated using four blood test results - bilirubin, serum sodium, INR and serum creatinine. Your care team will notify you of any major changes to your list status. You may have several changes to your score during your time on the wait list. When your updated blood work is delivered to your doctor, the transplant team will calculate your MELD score using an online calculator and submit the changes to UNOS directly. The results of your blood work are used to calculate your score for the waiting list. Since your health condition can change frequently, your doctor will send you to the lab for updated blood work routinely, so they can assess your condition often. The MELD score helps hospitals maintain fair lists across the nation so the livers that become available can go to those patients with the most urgent need. 
The MELD score was put into place so the sickest patients get the first livers available. The same MELD score definition and calculation are used by all transplant centers in the U.S.Īs of today, there are over 14,000 people waiting for a liver transplant, and there are not enough deceased donor livers to meet that need. The MELD score can range from 6 (less ill) to 40 (gravely ill). It’s used by hospitals and the government to prioritize allocation of deceased donor livers for transplant. MELD is an acronym for model for end-stage liver disease, and MELD score is the score provided to patients based on how urgently they need a liver transplant in the next three months. We’ve put together this blog post to help answer the most frequently asked questions about the MELD score. Having a strong understanding of your MELD score and how it’s calculated is important because it often influences how long you’ll wait for your liver transplant. If you’re a liver transplant patient, you’ve likely heard your doctors talk about your MELD score. On-Treatment Improvement of MELD Score Reduces Death and Hepatic Events in Patients With Hepatitis B-Related Cirrhosis. Yip TC, Chan HL, Tse YK, Lam KL, Lui GC, Wong VW, et al. 
University of Wisconsin School of Medicine and Public Health. Model for End-stage Liver Disease (MELD) score and liver transplant: benefits and concerns. doi:10.2147/CEG.S160537Īiello FI, Bajo M, Marti F, Gadano A, Musso CG. Liver function tests in identifying patients with liver disease. Correction factor to improve agreement between point-of-care and laboratory International Normalized Ratio values. Johnson SA, Vazquez SR, Fleming R, Lanspa MJ. Analysis of mortality prognostic factors using model for end-stage liver disease with incorporation of serum-sodium classification for liver cirrhosis complications: A retrospective cohort study. The impact of cirrhosis and MELD score on postoperative morbidity and mortality among patients selected for liver resection. Zaydfudim VM, Turrentine FE, Smolkin ME, et al. Evaluation of model performance to predict survival after transjugular intrahepatic portosystemic shunt placement. Important predictor of mortality in patients with end-stage liver disease. Management of patients with liver diseases on the waiting list for transplantation: a major impact to the success of liver transplantation.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |



 RSS Feed
RSS Feed
